Speech and the Brain
Dr. C. George Boeree
Lateralization
The brain is divided into two halves, a left hemisphere and a right hemisphere. This is called lateralization, and applies to any animal further up the evolutionary tree than, say, a worm. In animals that are particularly vocal, such as canaries, dolphins, and chimpanzees, it seems that one hemisphere or another is dedicated to controlling those behaviors and the responses to them.
In human beings, it is the left hemisphere that usually contains the specialized language areas. While this holds true for 97% of right-handed people, about 19% of left-handed people have their language areas in the right hemisphere and as many as 68% of them have some language abilities in both the left and the right hemispheres.
Lateralization was first discovered in the 1800's by physicians (such as Broca and Wernicke, who we will discuss in a bit) who did autopsies on patients who had had several language difficulties before their deaths. These physicians found damage to particular areas of the brain now named after them, and these areas were consistently on the left hemisphere.
These discoveries were later confirmed in the 1950's by researchers, such as Wilder Penfield and Herbert Jasper. Brain surgery is normally done using only local anesthesia. The patient is sedated but not unconscious. This is done in part in order to be able to keep tabs on the patient's experiences. Penfield and Jasper took advantage of these patients (with their permission, of course) and stimulated certain areas electrically. When asked questions, the patients were unable to reply during te stimulation of the left hemisphere, but had no problem responding during stimulation of the right hemisphere.
In the 1960's, another, rather bizarre, set of experiments involved using sodium amytal, a very fast-acting anesthetic. Researchers were able to put one or the other hemisphere of volunteers to sleep by injecting the anesthetic into either the right or left carotid artery (which supply blood to the same-side hemispheres). Lo and behold, the patients who had the left hemisphere put to sleep did not respond to questions!
Most recently, researchers have taken advantage of the huge advances made in brain imaging. In particular, the PET scan ("positron emission tomography") provides a computer with the information needed to construct a three dimensional map of a persons brain including the relative activity of different areas. PET scans involve injecting someone with a radioactive glucose solution. Since active areas of the brain use more energy, and therefore more glucose, they release more radiation, which the computer translates into "warmer" colors such as yellow and red. Areas that are less active are shown with "cooler" colors such as green and blue. As by now you should expect, certain areas of the left hemisphere were more active while people were engaged in linguistic activities.
Most early studies were done on mature male volunteers. Since then, scientists have gone on to study female volunteers and even children. Interestingly, women seem to be slightly less "lateralized" than men, being more likely to use portions of the right hemisphere as well as the left.
Studies of children have provided some fascinating information: If a child has damage to the left hemisphere, the child may develop language in the right hemisphere instead. The younger the child, the better the recovery. So, although the "natural" tendency is for language to develop on the left, our brains are capable of adapting to difficult circumstances, if the damage occurs early enough.
Broca's Area
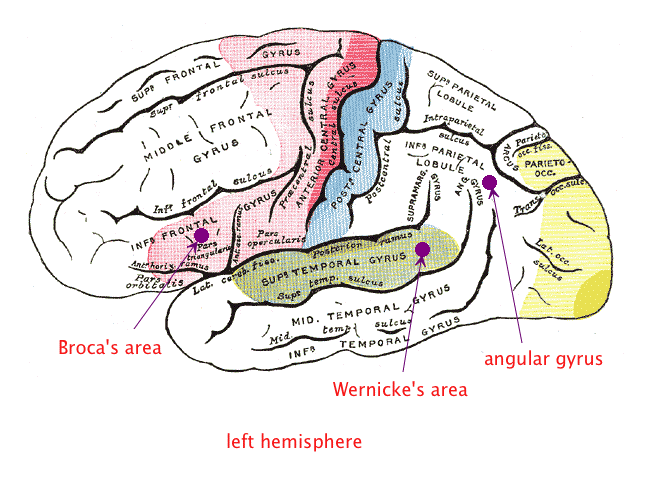
The first language area within the left hemisphere to be discovered is called Broca's Area, after Paul Broca. Broca was a French neurologist who had a patient with severe language problems: Although he could understand the speech of others with little difficulty, the only word he could produce was "tan." Because of this, Broca gave the patient the pseudonym "Tan." After the patient died, Broca performed an autopsy, and discovered that an area of the frontal lobe, just ahead of the motor cortex controlling the mouth, had been seriously damaged. He correctly hypothesized that this area was responsible for speech production.
Physicians called the inability to speak aphasia, and the inability to produce speech was therefore called Broca's aphasia, or expressive aphasia. Someone with this kind of aphasia has little problem understanding speech. But when trying to speak themselves are capable only of slow, laborious, often slurred sequences of words. They don't produce complete sentences, seldom use regular grammatical endings such as -ed for the past tense, and tend to leave out small grammatical words.
It turns out that Broca's area is not just a matter of getting language out in a motor sense, though. It seems to be more generally involved in the ability to deal with grammar itself, at least the more complex aspects of grammar. For example, when they hear sentences that are put into a passive form, they often misunderstand: If you say "the boy was slapped by the girl," they may understand you as communicating that the boy slapped the girl instead.
Wernicke's Area
The second language area to be discovered is called Wernicke's Area, after Carl Wernicke, a German neurologist. Wernicke had a patient who could speak quite well, but was unable to understand the speech of others. After the patient's death, Wernicke performed an autopsy and found damage to an area at the upper portion of the temporal lobe, just behind the auditory cortex. He correctly hypothesized that this area was responsible for speech comprehension.
This kind of aphasia is known as Wernicke's Aphasia, or receptive aphasia. When you ask a person with this problem a question, they will respond with a sentence that is more or less grammatical, but which contains words that have little to do with the question or, for that matter, with each other. Strange, meaningless, but grammatical sentences come forth, a phenomenon called "word salad."
Like Broca's area is not just about speech production, Wernicke's is not just about speech comprehension. People with Wernicke's Aphasia also have difficulty naming things, often responding with words that sound similar, or the names of related things, as if they are having a very hard time with their mental "dictionaries."
Other Areas
Despite the fact that Broca's and Wernicke's Areas are in different lobes, they are actually quite near each other and intimately connected by a tract of nerves called the arcuate fascilicus. There are also people who have damage to the arcuate fascilicus, which results in an aphasia known as conduction aphasia. These people have it a bit better than other aphasias: They can understand speech, and they can (although with difficulty) produce coherent speech, they cannot repeat words or sentences that they hear.
Reading and writing are a part of language as well, of course. But since these skills have only been around a few thousand years, they are not as clearly marked in terms of brain functioning as the basic comprehension and production areas. But there is an area of the brain called the angular gyrus that lies about halfway between Wernicke's area and the visual cortex of the occipital lobe. It was discovered, after a young patient with reading problems died and his brain was examined during autopsy. The angular gyrus showed significant abnormalities.
The angular gyrus has been implicated in problems such as alexia (the inability to read), dyslexia (difficulties with reading), and agraphia (the inability to write). In research involving the use of PET scans on people with these problems, the angular gyrus is not as active as it is in other people while engaged in reading or writing. However, problems such as dyslexia also can involve other areas of the brain, or not involve brain disorders at all.
Dr. C. George Boeree
Lateralization
The brain is divided into two halves, a left hemisphere and a right hemisphere. This is called lateralization, and applies to any animal further up the evolutionary tree than, say, a worm. In animals that are particularly vocal, such as canaries, dolphins, and chimpanzees, it seems that one hemisphere or another is dedicated to controlling those behaviors and the responses to them.
In human beings, it is the left hemisphere that usually contains the specialized language areas. While this holds true for 97% of right-handed people, about 19% of left-handed people have their language areas in the right hemisphere and as many as 68% of them have some language abilities in both the left and the right hemispheres.
Lateralization was first discovered in the 1800's by physicians (such as Broca and Wernicke, who we will discuss in a bit) who did autopsies on patients who had had several language difficulties before their deaths. These physicians found damage to particular areas of the brain now named after them, and these areas were consistently on the left hemisphere.
These discoveries were later confirmed in the 1950's by researchers, such as Wilder Penfield and Herbert Jasper. Brain surgery is normally done using only local anesthesia. The patient is sedated but not unconscious. This is done in part in order to be able to keep tabs on the patient's experiences. Penfield and Jasper took advantage of these patients (with their permission, of course) and stimulated certain areas electrically. When asked questions, the patients were unable to reply during te stimulation of the left hemisphere, but had no problem responding during stimulation of the right hemisphere.
In the 1960's, another, rather bizarre, set of experiments involved using sodium amytal, a very fast-acting anesthetic. Researchers were able to put one or the other hemisphere of volunteers to sleep by injecting the anesthetic into either the right or left carotid artery (which supply blood to the same-side hemispheres). Lo and behold, the patients who had the left hemisphere put to sleep did not respond to questions!
Most recently, researchers have taken advantage of the huge advances made in brain imaging. In particular, the PET scan ("positron emission tomography") provides a computer with the information needed to construct a three dimensional map of a persons brain including the relative activity of different areas. PET scans involve injecting someone with a radioactive glucose solution. Since active areas of the brain use more energy, and therefore more glucose, they release more radiation, which the computer translates into "warmer" colors such as yellow and red. Areas that are less active are shown with "cooler" colors such as green and blue. As by now you should expect, certain areas of the left hemisphere were more active while people were engaged in linguistic activities.
Most early studies were done on mature male volunteers. Since then, scientists have gone on to study female volunteers and even children. Interestingly, women seem to be slightly less "lateralized" than men, being more likely to use portions of the right hemisphere as well as the left.
Studies of children have provided some fascinating information: If a child has damage to the left hemisphere, the child may develop language in the right hemisphere instead. The younger the child, the better the recovery. So, although the "natural" tendency is for language to develop on the left, our brains are capable of adapting to difficult circumstances, if the damage occurs early enough.
Broca's Area
The first language area within the left hemisphere to be discovered is called Broca's Area, after Paul Broca. Broca was a French neurologist who had a patient with severe language problems: Although he could understand the speech of others with little difficulty, the only word he could produce was "tan." Because of this, Broca gave the patient the pseudonym "Tan." After the patient died, Broca performed an autopsy, and discovered that an area of the frontal lobe, just ahead of the motor cortex controlling the mouth, had been seriously damaged. He correctly hypothesized that this area was responsible for speech production.
Physicians called the inability to speak aphasia, and the inability to produce speech was therefore called Broca's aphasia, or expressive aphasia. Someone with this kind of aphasia has little problem understanding speech. But when trying to speak themselves are capable only of slow, laborious, often slurred sequences of words. They don't produce complete sentences, seldom use regular grammatical endings such as -ed for the past tense, and tend to leave out small grammatical words.
It turns out that Broca's area is not just a matter of getting language out in a motor sense, though. It seems to be more generally involved in the ability to deal with grammar itself, at least the more complex aspects of grammar. For example, when they hear sentences that are put into a passive form, they often misunderstand: If you say "the boy was slapped by the girl," they may understand you as communicating that the boy slapped the girl instead.

Wernicke's Area
The second language area to be discovered is called Wernicke's Area, after Carl Wernicke, a German neurologist. Wernicke had a patient who could speak quite well, but was unable to understand the speech of others. After the patient's death, Wernicke performed an autopsy and found damage to an area at the upper portion of the temporal lobe, just behind the auditory cortex. He correctly hypothesized that this area was responsible for speech comprehension.
This kind of aphasia is known as Wernicke's Aphasia, or receptive aphasia. When you ask a person with this problem a question, they will respond with a sentence that is more or less grammatical, but which contains words that have little to do with the question or, for that matter, with each other. Strange, meaningless, but grammatical sentences come forth, a phenomenon called "word salad."
Like Broca's area is not just about speech production, Wernicke's is not just about speech comprehension. People with Wernicke's Aphasia also have difficulty naming things, often responding with words that sound similar, or the names of related things, as if they are having a very hard time with their mental "dictionaries."
Other Areas
Despite the fact that Broca's and Wernicke's Areas are in different lobes, they are actually quite near each other and intimately connected by a tract of nerves called the arcuate fascilicus. There are also people who have damage to the arcuate fascilicus, which results in an aphasia known as conduction aphasia. These people have it a bit better than other aphasias: They can understand speech, and they can (although with difficulty) produce coherent speech, they cannot repeat words or sentences that they hear.
Reading and writing are a part of language as well, of course. But since these skills have only been around a few thousand years, they are not as clearly marked in terms of brain functioning as the basic comprehension and production areas. But there is an area of the brain called the angular gyrus that lies about halfway between Wernicke's area and the visual cortex of the occipital lobe. It was discovered, after a young patient with reading problems died and his brain was examined during autopsy. The angular gyrus showed significant abnormalities.
The angular gyrus has been implicated in problems such as alexia (the inability to read), dyslexia (difficulties with reading), and agraphia (the inability to write). In research involving the use of PET scans on people with these problems, the angular gyrus is not as active as it is in other people while engaged in reading or writing. However, problems such as dyslexia also can involve other areas of the brain, or not involve brain disorders at all.

